Part 1: Pre-Implant Process
Tooth loss is a growing global issue. It affects an individual's ability to eat and speak normally and has a substantial negative impact on one’s smile and facial esthetics. Besides, tooth loss can also cause premature facial changes that can make one look older than they actually are. According to the American College of Prosthodontists, over 178 million Americans are missing at least one natural tooth. The problem is exacerbated with age; around 30% of US adults aged between 65-74 have lost all their teeth, either because of dental trauma, periodontal infection, or tooth decay.
When it comes to replacing missing natural teeth, several options are available. Conventionally, dentists used removable dentures or fixed teeth bridges for tooth replacement. However, each option has its own merits and demerits, the most prominent drawbacks being their limited clinical lifespan and incomplete restoration of dental functions.
Then came dental implants - a revolutionary, lifelong, and esthetically pleasing solution for missing teeth. Today, dental implants have become the most preferred replacement option for missing teeth across the globe. If you are thinking about replacing your missing teeth but you’re wondering if dental implants are the right choice for you, we have prepared a comprehensive guide that offers everything you need to know about dental implants.
What are Dental Implants?
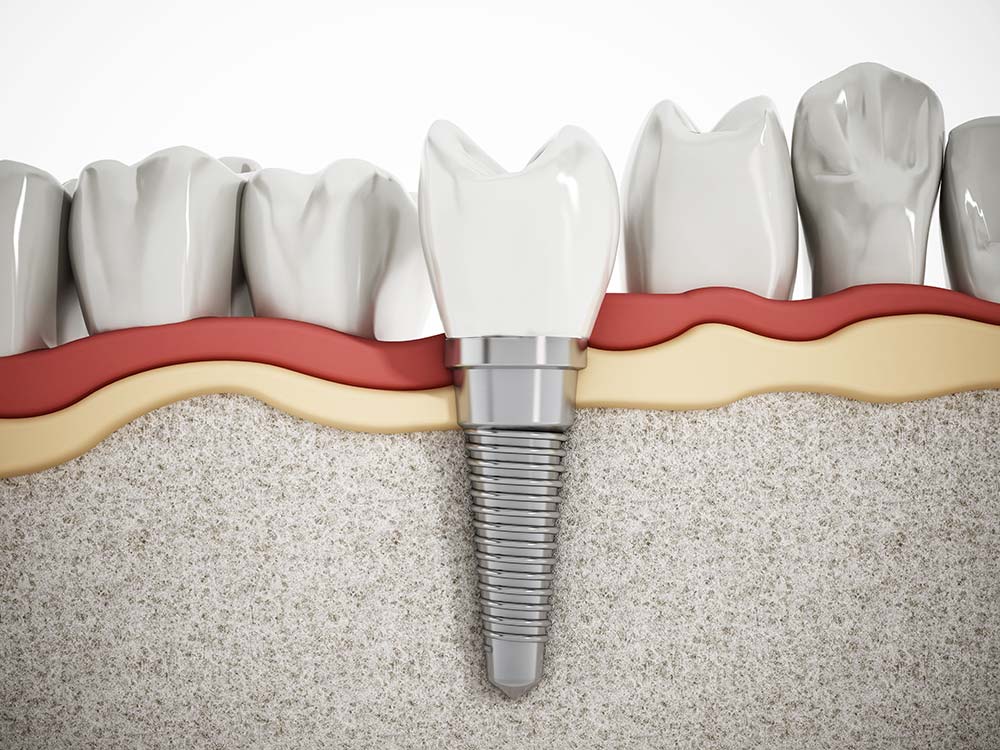
According to the American Dental Association, a dental implant is a cylindrical fixture inserted into the jawbone and functions as an artificial tooth root. Dental implants are made from titanium and are surgically inserted into the jawbone.
Over time, bone tissue starts to grow around the implants that ensure they remain firmly anchored and support any prosthesis - whether an overdenture, fixed complete bridge or a dental crown is attached over it - remains firmly stable and allows optimal dental function.
How Do Dental Implants Work?
Have you ever wondered why dental implants have such a high success rate? The success of titanium-based dental implants is their ability to promote healthy and strong bone formation around the implants. This process, known as osseointegration, forms the basis of dental implants’ ability to support artificial teeth and restore optimal dental function. So, the higher is the osseointegration, the more firmly the implant will be embedded within the jawbone to support artificial teeth.
Are Implants the best option?
According to the American Academy of Implant Dentistry, any individual with good oral and physical health, who has lost one more tooth, is a candidate for getting implants. However, the most crucial requirement for getting implants is sufficient healthy bone tissue to hold the implants and their attached artificial teeth.
During the initial appointment, your dentist will thoroughly assess your oral health status and take X-ray images of your teeth and jaws to evaluate the quality of the underlying bone. If sufficient bone tissue is not available, your dentist will perform additional surgical procedures like bone grafting or ridge augmentation to restore optimal bone density before placing the implants. These procedures are discussed in greater detail in the following sections.
Components of Dental Implants
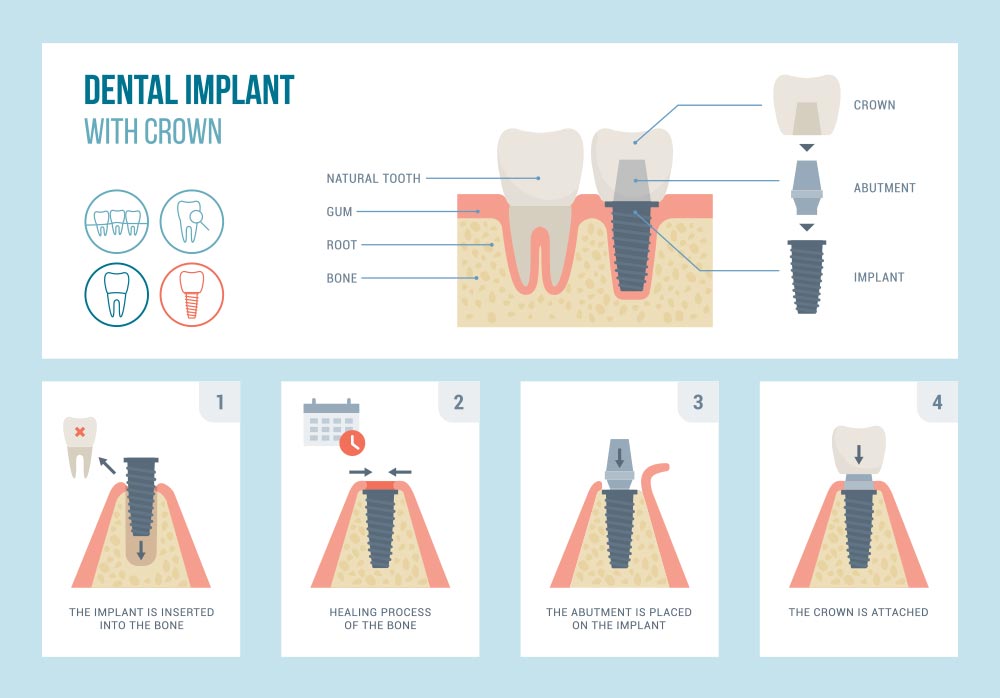
According to the American Association of Oral and Maxillofacial surgeons, an implant-supported artificial tooth consists of three components:
- Implant - this is the titanium post that serves as the replacement root
- Abutment - this is a component that fits over the implants and connects the artificial teeth to the implants substructure
- Prosthesis - depending on the number and location of the missing teeth, your dentist will attach a suitable prosthesis over one or more implants to complete the artificial tooth structure
Who Should Not Get Dental Implants?
While there are no absolute contraindications to getting dental implants, there are certain conditions that may temporarily make you an unsuitable candidate. However, as soon as these problems are resolved, you can get implants to replace your missing teeth. These conditions include:
How Many Teeth Can Dental Implants Replace?
Whether you have a single missing tooth or you have lost all your natural teeth, you can get them replaced with dental implants.
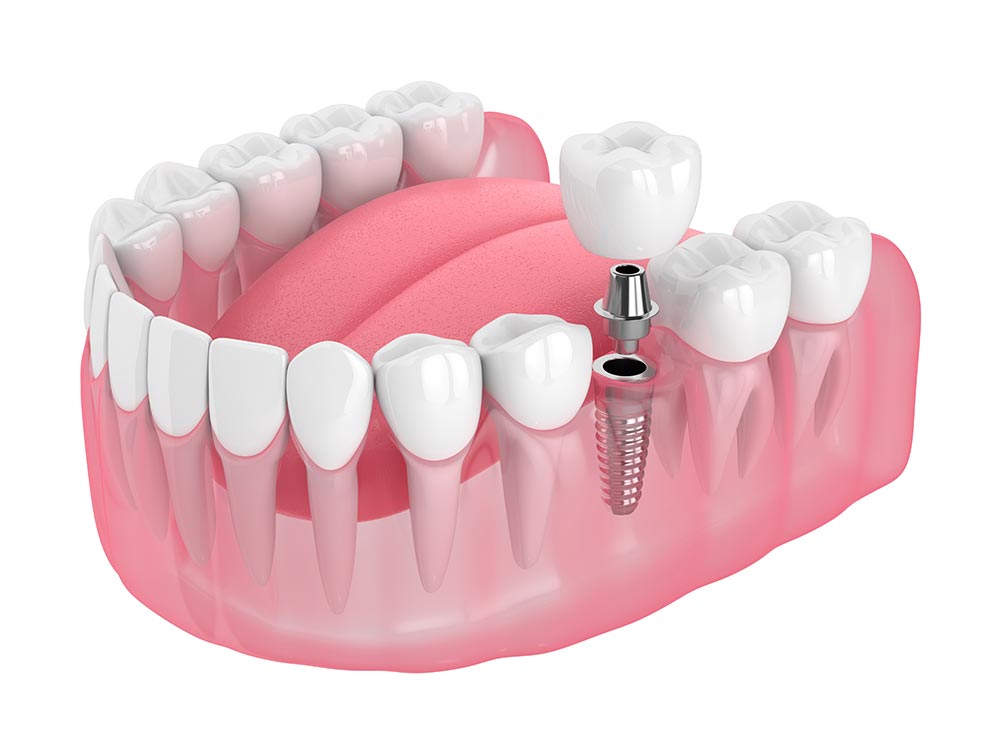
- Single Missing Tooth - if you just have one missing tooth, your dentist will replace it by placing an implant in place of the missing tooth and then restoring it with a zirconia crown.
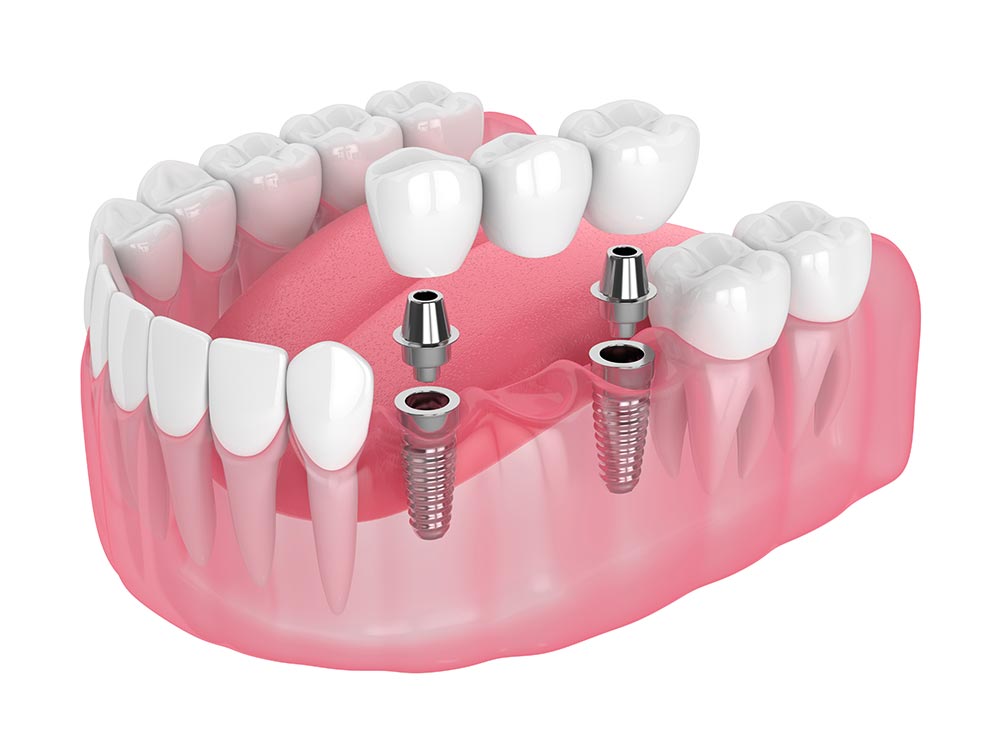
- Multiple Missing Teeth - if you have lost more than one tooth, your dentist may design an implant-supported overdenture for you. Unlike conventional dentures, implant-supported overdentures sit directly on the implants. Therefore, they are much more stable than traditional removable implants.
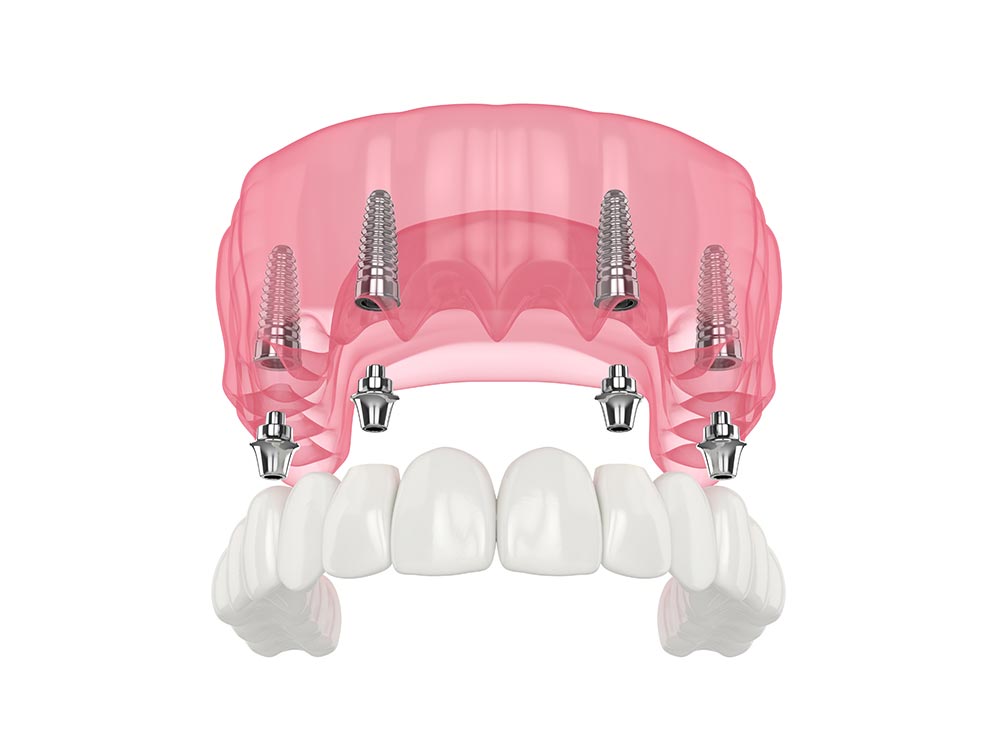
- Complete Tooth Loss - in case of complete tooth loss, your dentist will place up to four or six implants at pre-determined sites and use them for supporting a complete fixed bridge. These prostheses are known as all-on-four or six implant-supported fixed bridges. Unlike traditional teeth bridges that derive their support from the neighboring healthy teeth, the all-or supported fixed bridges are entirely supported by dental implants, making them considerably more durable and stable.
Dentists also use smaller implants, called mini-implants, for orthodontic purposes or in patients where sufficient vertical space is not available to place standard-length implants.
Why Should You Consider Dental Implants?
If you’re still not sure whether implants are the best option for you, here are some benefits of dental implants over other tooth replacement options:
- Strong and Durable - Titanium dental implants are highly strong and durable. As per the American Dental Association, tooth implants can last for a lifetime if they are cared for and looked after properly.
- Naturally Pleasing Esthetics - Dental implants allow your dentists to place esthetically pleasing prostheses, restoring your smile, facial esthetics, and self-confidence.
- Safety - Dental implants are made from titanium alloys, the safest materials to use inside the human body. Also, titanium implants have minimal allergic or other immunity-related adverse effects.
- Eat all your Favorite Foods - A drawback of conventional removable dentures is that they are not stable enough and allow one to eat hard or sticky foods. This problem has been eliminated with dental implants. Since the tooth implants are directly embedded into the jawbone like natural teeth, they firmly support the artificial teeth they support, allowing one to eat their favorite foods without any difficulty.
- No More Speech Problems - Denture wearers often have speech problems. We often come across denture wearers who have a distinct lisp in their voice and have difficulty pronouncing words. This is because they have to use their tongues to keep the dentures from slipping; besides, the dentures feel like a “foreign object” inside the mouth and make word pronunciation difficult. On the other hand, dental implants do not take extra space in the mouth and are firmly anchored. So, they restore your ability to speak without difficulty.
- Tooth Conservation - Conventional dentures and bridges often require sacrificing natural tooth structure for their attachment/insertion. As a result, these supporting teeth become more prone to the development of tooth decay, and some even fracture under constant pressure. Since the implants are placed inside the bone, they don’t require any supporting teeth and hence, do not require sacrificing natural tooth enamel.
- Jawbone Conservation - Conventional dentures rest on the oral soft tissues and jawbone for stability and retention. That is why prolonged denture use puts direct pressure on the underlying bone, which starts to degrade at a faster rate. According to the American Association of Oral and Maxillofacial Surgeons, this can lead to premature wrinkling of the face due to bone resorption. Besides, bone resorption also makes the jaws brittle, weak, and more prone to fracture. Dental implants, on the other hand, do not cause bone resorption. Instead, they promote new bone formation through osseointegration and prevent premature facial structural changes.
Now that we understand what dental implants are and how they work, let’s understand the steps involved in implant treatment planning, placement, and aftercare.
Part 2: The Implant Procedure
In part-I of this guide, we discussed the basics of dental implantology: what are dental implants, who can benefit from them, and most importantly, their advantages. In part II, we discuss the implant placement procedure in detail.
The Dental Implant Procedure
The placement of dental implants is an intricate procedure that requires surgical skills and expertise. That is why it is usually performed in various steps. The idea is to prepare a customized treatment plan that offers the best esthetic and clinical outcomes while minimizing complications and adverse effects.
1. Pre-Surgical Appointment
During your first sitting, your dentist will perform a thorough examination of your teeth and overall dental health. They will examine the status of your existing teeth and evaluate options for their replacement. They will also look for any underlying conditions that may affect the outcome of your treatment such as periodontal inflammation, bone disease, or teeth cavities.



2. Treatment Planning
Besides a clinical examination, your dentist will also perform various diagnostic tests to prepare a treatment plan that is customized according to your dental needs.
- Tooth Models - your dentist will make impressions of your teeth to prepare tooth models. These models will be used for identifying the most suitable prosthesis that should be used for tooth replacement with dental implants.
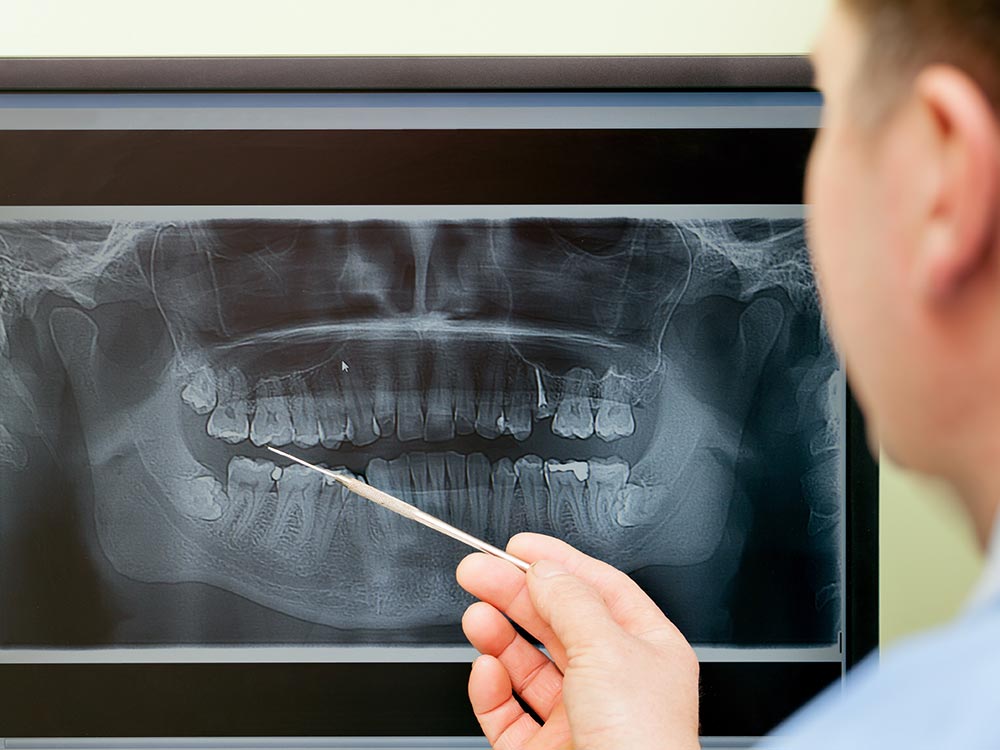
- Digital X-Ray Images - your dentist will take x-ray images of your teeth and the region where the teeth are missing. This is done to visualize the quality and health of the underlying bone. It is also done to identify any important anatomical landmarks like nerves, blood vessels, or the air sinuses that may in the region of implant surgery.
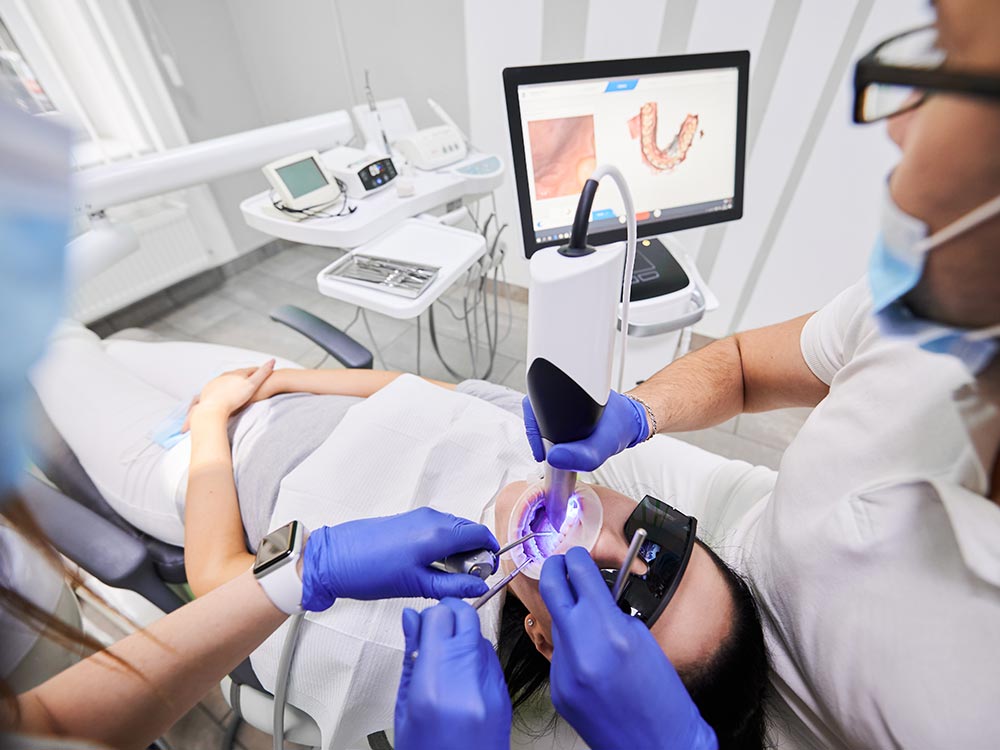
- Intra-oral Imaging - your dentist may also use an intra-oral camera to show you the status of your existing teeth and gums. Normally, dentists use intra-oral cameras for educating the patients about any possible complexities that may require additional procedures like teeth fillings or extractions before implant placement.
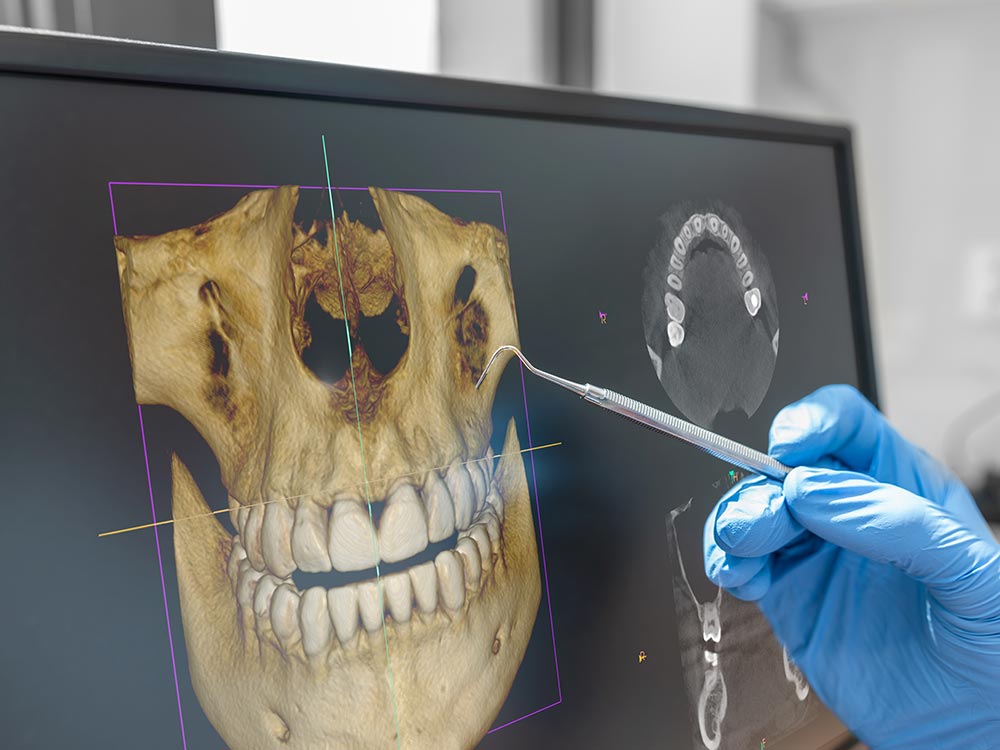
- 3D Imaging - today, dentists rely on 3D imaging technology - cone-beam computed tomography (CBCT) - helping the dentist visualize thin slices of the facial structure and allows to precisely locate the most favorable position and angulation of the implants. CBCT imaging allows dentists to assess the health of the underlying bone. If there is insufficient jawbone available to support the implant, they may suggest a bone graph.

- Implant Surgical Guide - the surgical guide is a template that guides the dentist in inserting the implants at the precise, pre-determined site. Research has shown that surgical guides considerably improve the clinical outcome of dental implant therapy.
3. Pre-Surgical Treatment
During the clinical examination, if your dentist identifies any underlying issue, they will remove it first before proceeding with the implant surgery. As discussed previously, if there is underlying jawbone inflammation, it can adversely affect the success of implant therapy. Therefore, your dentist will first perform deep scaling and root planning to remove the plaque and tartar deposits. Similarly, if there are any teeth cavities in the existing teeth, the affected teeth will be restored with a suitable filling material before beginning the implant process. If a tooth cannot be salvaged, your dentist will remove it as well and replace it with an implant-supported prosthesis.
The most critical factor that determines the success of dental implants is the health and density of the jawbone that will support the implant. If your dentist feels that sufficient bone is not available to support the implant, they will restore the bone quality by performing various surgical procedures.
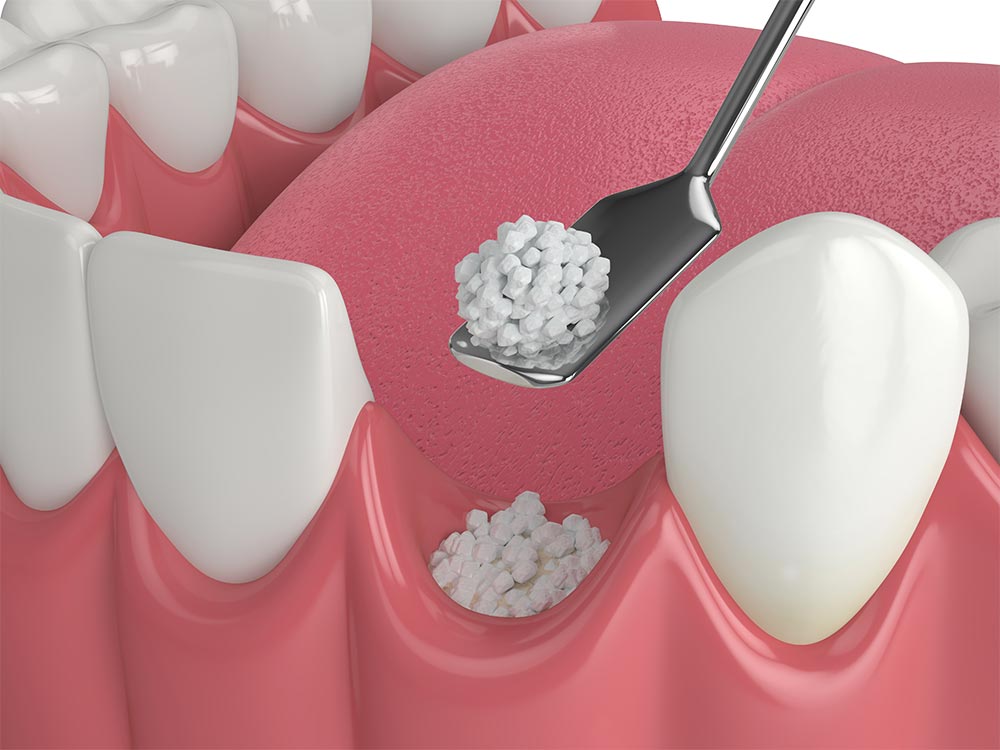
- Bone Grafting - according to the American Academy of Implant Dentistry, a bone graft is a surgical procedure in which your dentist will replenish the desired density of the jawbone with a bone graft taken from natural or artificial sources. The choice of using a natural or artificial bone graft depends on various factors, such as the extent of bone deficiency, general health conditions, and the body’s immune response. Since bone grafting is a surgical procedure, it is performed under the effect of anesthesia.
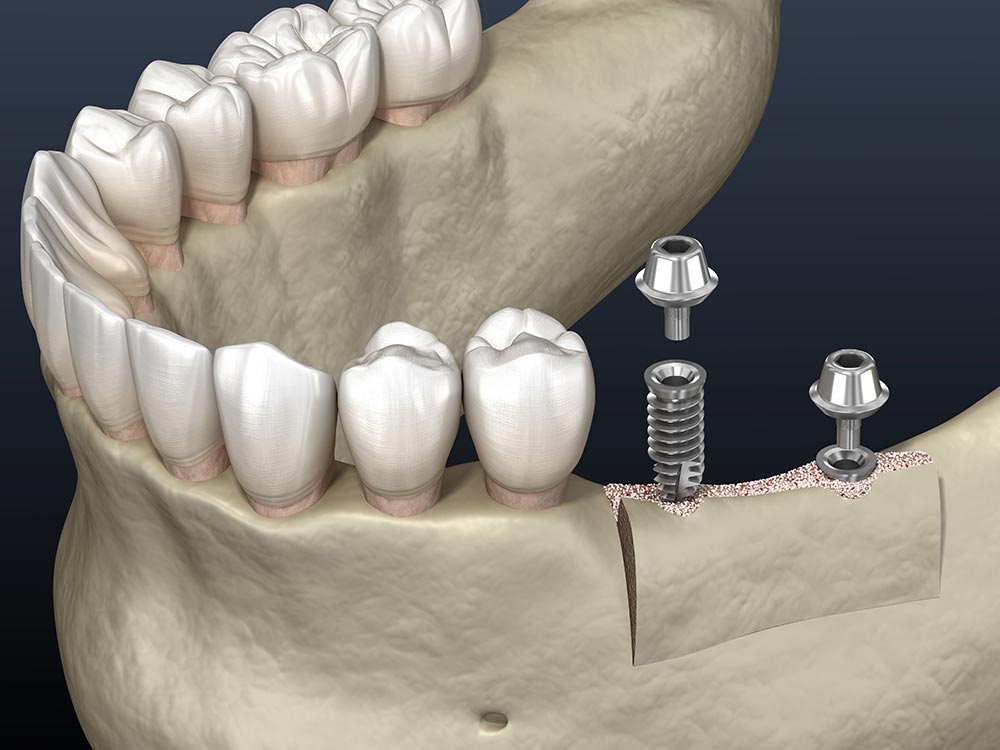
- Ridge Augmentation - the part of the bone that supports our teeth is known as the alveolar bone. Under healthy conditions, the top-most part, or the ridge of the alveolar bone appears rounded. A rounded alveolar ridge not only indicates a healthy bone but also provides sufficient support for the implant. Unfortunately, the alveolar ridge undergoes rapid resorption following the extraction or loss of a tooth. Ultimately, the alveolar ridge becomes thin and is unfavorable for implant insertion. In these cases, your dentist will recontour the alveolar ridge with a suitable bone graft.
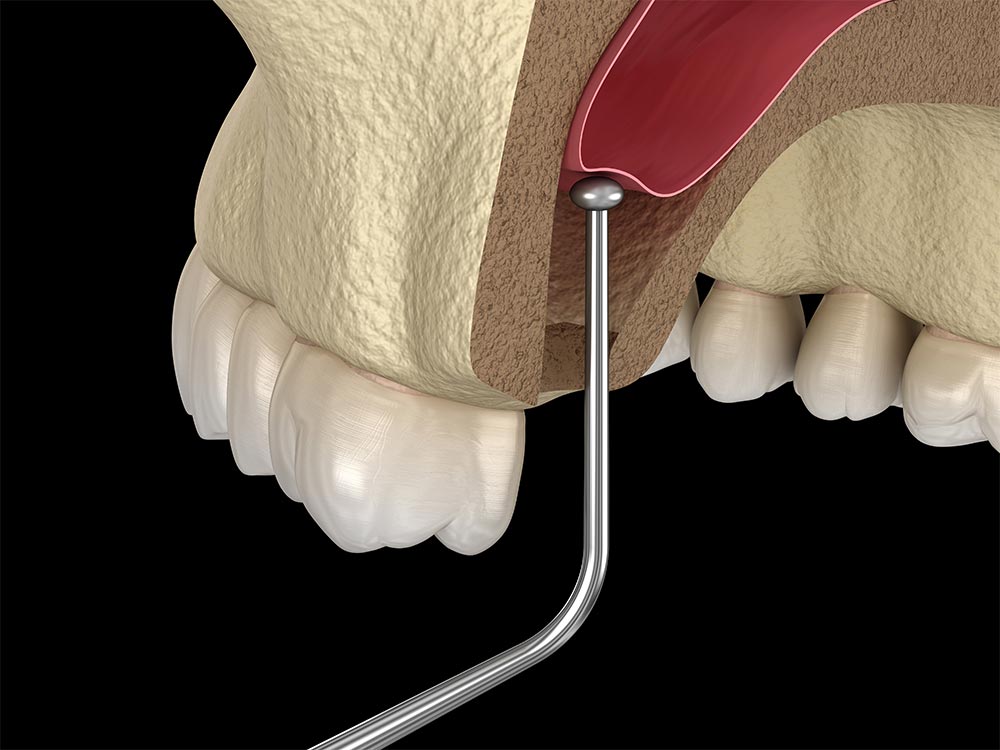
- Sinus Lift Procedure - our facial and head region contains various air-filled spaces that help in maintaining the qualify of our voice and to reduce the overall weight of the head. One such pair of sinuses is also present in the upper jaws. If the upper back teeth are lost prematurely, it can lead to excessive bone resorption, causing the sinus to slide downwards. If the maxillary sinuses extend too downward, there may not be enough bone tissue left between the sinus floor and the jawbone to support an implant. In these cases, dentists perform a sinus lift procedure. According to the American Academy of Periodontology. A sinus lift refers to a procedure in which the sinus floor is raised and a bone graft is added into the space to reinforcing the jawbone. This prevents any serious, even life-threatening medical complication which might have occurred if the implant accidentally pierces the sinus’s floor or membrane.
Since these are surgical procedures, you will have to wait approximately four to six months for the surgical site to heal before the implant placement procedure can be initiated.
4. Surgical Procedure
Now that all the underlying issues have been addressed, your dentist will now focus on the implant insertion.
Administration of Anesthesia
Since this is a surgical procedure, your dentist will perform it under the effect of anesthesia. Depending on the expected duration of the procedure, the number of implants to be placed, and the anxiety of level of the patients, dentists use various types of anesthesia.
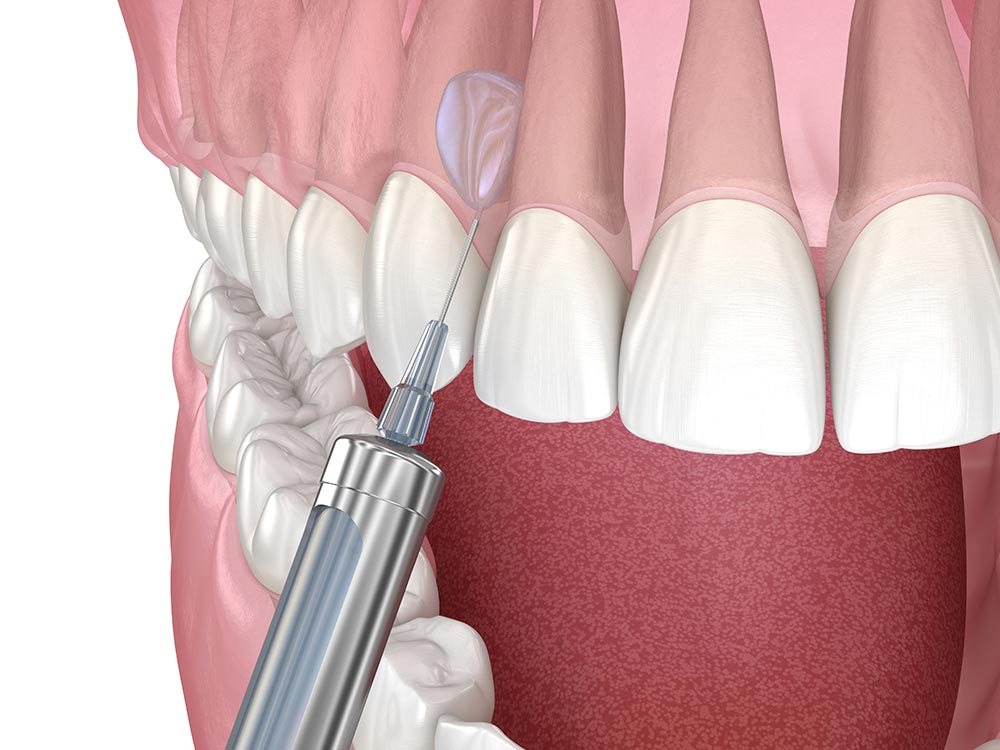
- Local Anesthesia - dentists routinely perform dental implant insertion procedures at the dental chairside using local anesthesia. In this type of anesthesia, only the region where the implant is to be inserted is numbed. The effect of local anesthesia may last for a few hours after the procedure. You should avoid eating anything until the anesthesia’s effect fades off completely.

- Conscious Sedation - for extremely apprehensive or anxious patients who are afraid of dental treatment, dentists make them calm and relaxed by performing the procedure under sedation. In conscious sedation, the patient remains in a relaxed, drowsy state but is still conscious enough to respond to the dentist’s verbal instructions. The various levels of sedation are as follows:
- Inhalation Sedation - this is the simplest form of sedation and involves asking the patient to wear and breath through a mask that contains a mixture of oxygen and nitrous oxide. Nitrous oxide, also called the laughing gas not only relieves pain but also puts the patient under low-level sedation.
- Oral Sedation - this type of sedation puts patients under a deep sleep. Your dentist will prescribe you oral sedatives that are to be taken one hour before the appointment. Oral sedation is usually reserved for uncooperative and frightened patients.
- IV Sedation - in this type of sedation, patients are put to deep sleep by injecting an intravenous sedative. IV sedation is usually reserved for patients where a number of procedures are to be performed in a single sitting.
Dentists have to undergo additional training to perform procedures under sedation. Besides, an anesthetist needs to be present at all times to monitor the patient’s vital signs during the procedure and in the post-operative recovery phase. In some cases, dentists may choose to perform dental procedures under general anesthesia - in the case of physically or mentally challenged, or extremely apprehensive or phobic patients.
Implant Insertion
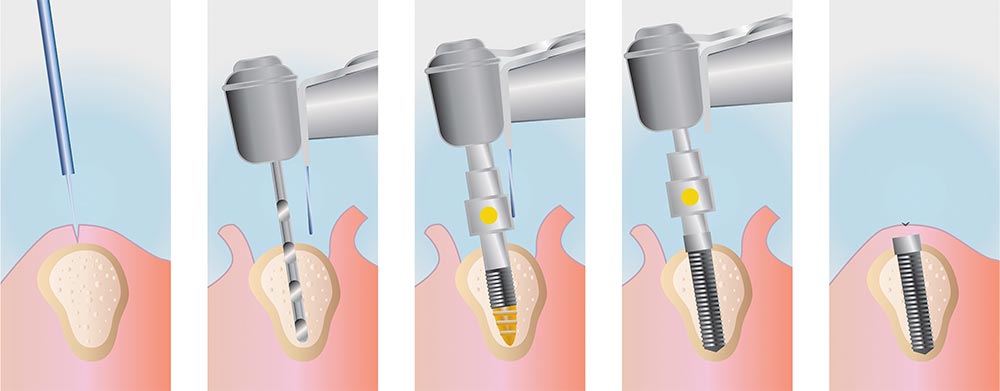
Once the anesthesia has been administered and you are relaxed and pain-free, your dentist will begin the insertion procedure. First, your dentist will make an insertion over the soft tissue to expose the underlying jawbone where the implant will be inserted. Next, a surgical flap will be raised followed by drilling a hole inside the bone. The diameter of the hole will be adjusted so that it is slightly narrower than the width of the implant. In the next step, your dentist will use controlled forces to carefully screw the implant into its position. Great care is taken not to apply excessive forces as it may damage the surrounding bone and affect implant outcome. In this way, your dentist will insert all the implants in their pre-determined locations.
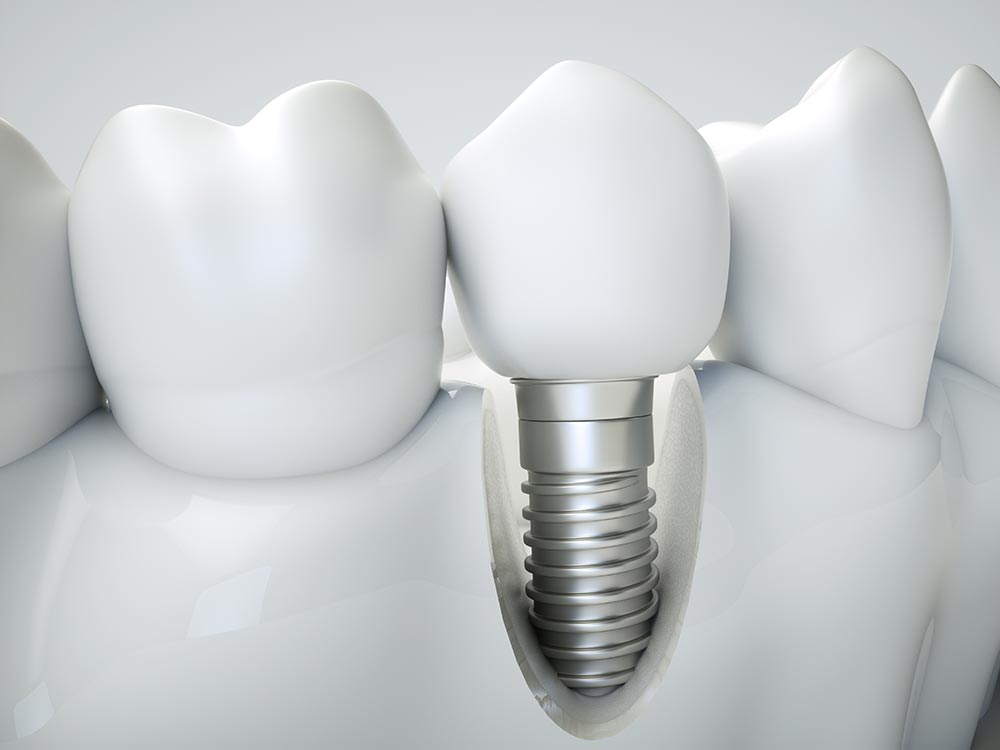
- Once an implant is inserted into the bone, your dentist will place a healing collar over it. The purpose of this collar is to protect the underlying implant from excessive loads or unwanted movements, which may compromise the process of osseointegration. Finally, your dentist will suture back the surgical flap to its position to complete the implant surgery.
If the implant surgery was performed under local anesthesia or inhalation sedation, then you can go home right away. However, if your surgery was performed under oral or IV sedation, your dentist will keep you in the recovery room for some time - to ensure that your vital signs are stable and there is no adverse effect from the sedative. Patients who are treated under oral or IV sedation are not allowed to drive themselves, or to resume work until the following day - especially if their job requires attention or precision.
Implant Loading
Implant loading is a process in which your dentist will attach a suitable prosthesis over the implants once they have become firmly embedded in the bone.
- Delayed Implant Loading - generally, dentists wait four to six months before implants are loaded with a prosthesis. During this time, your dentist will attach a temporary restoration over the implants so that your facial esthetics are not affected while you wait for healing to occur. However, these temporary restorations are only for esthetics purposes, and you cannot use them for eating. This type of implant loading is known as immediate implant loading.
- Immediate Implant Loading - in some cases, dentists may also load implants with a prosthesis immediately after their insertion. However, this type of implant loading is not commonly performed since not all patients are suitable candidates.
Congratulations!
You are now the proud owner of an attractive and healthy smile with your new dental implant.
Part 3: Aftercare
In the previous two parts of this guide, we discussed how dental implants work and the procedure involved in getting them. In part III, we will discuss how to look after your implant-supported teeth to maximize their life and ensure optimal esthetics.
Getting your teeth replaced with dental implants is the easy part. But maintaining your implant-supported teeth throughout life requires optimal oral hygiene maintenance and adherence to your dentist’s instructions. This section offers simple tips that can help you ensure a healthy oral cavity and a set of pearly white teeth.
What to Expect After Getting a Dental Implant?
Can I Drive Myself Home After the Procedure?
If your implant surgery was performed under intravenous sedation, your dentist would ask you to rest in the recovery room for some time. This is to ensure that your vitals are normal, and you’re all ready to go home. While it may be possible for you to drive yourself home after getting treated under inhalation sedation, individuals who receive treatment under oral or IV sedation remain drowsy for a prolonged duration.
Hence, they are not allowed to drive themselves home. Instead, your dentist will ask you to be accompanied by a caretaker or a loved one who can drive you back home.
Can I Resume Work Immediately After the Surgery?

If you have been treated with local anesthesia or inhalation sedation, the effects of the anesthetic and nitrous oxide quickly wear off. As a result, you can return to your office after the surgery. However, you should not operate any heavy machinery for a few hours after the procedure. If your treatment was performed under oral or IV sedation, you should not go back to work. Instead, you should be accompanied home, and you should rest for the entire day.
Is Pain/Swelling Normal After the Implant Procedure?
Dental implants are inserted into the jawbone through a surgical procedure. Hence, it is normal to have slight pain and swelling around the surgical site. Your dentist may prescribe painkillers to subside the pain and swelling. You may also apply ice packs on the affected side of the face or rinse the affected side with lukewarm saline water.
Both these measures will help in containing the inflammation and reducing the swelling. More importantly, you should avoid smoking as it can adversely affect the healing process.
In some cases, they may also prescribe antibiotics to prevent infection. Nevertheless, the swelling should go away in a few days or weeks as the surgical site continues to heal.
Is it Normal for the Surgical Site to Bleed?
Minor, transient bleeding from the surgical site is perfectly normal for the first few days. Afterward, a clot will form around the implant site, and the bleeding should stop. This clot plays an important role in the healing of the implant site as it is ultimately converted into bone tissue and other cells that are essential for the healing process. Therefore, every effort must be made to preserve the blood clot. If bleeding does not stop after a few days, it is cause for concern, and you should visit your dentist immediately for advice.
How to Look After Implant-supported Teeth?
Initial Diet Management
Immediately after the implant surgery, you should take on a soft food diet for the first few days, even if you have received a temporary restoration. The provisional restorations are for restoring the facial esthetics and not for eating. Gradually, you can shift to semi-solid foods while eating from the non-affected side. This is to ensure that the implant-surgical site heals without any disturbance.
Furthermore, avoid drinking anything with a straw as it may put pressure on the surgical site and may lead to the dislodgment of the clot, thereby delaying the healing process.
Once the implant site has completely healed, and your dentist has attached the permanent restoration over the implant, you can resume your normal diet. Once the implants have been loaded, there is no diet restriction - you can eat all your favorite foods without any worry about implant prosthesis dislodgment.
Oral Hygiene Maintenance
The most important aspect in enhancing the clinical survival of implant-supported teeth is ensuring optimal oral hygiene. The American Dental Association recommends brushing at least twice a day and flossing once daily to keep the implant sites clean and plaque-free. Your dentist may also recommend a special toothbrush and mouthwash to prevent tooth cavities and bacterial growth.
Regular Dental Visits
According to the American Dental Association, regular dental checkup visits go a long way in ensuring the long-term survival of implant-supported teeth. This is because dentists use specialized equipment to detect underlying problems with your natural or implant-supported teeth well before they become visible to the naked eye. As a result, they can treat these developing problems before they lead to an adverse effect on your oral health, or cause implant failure.
When should I visit my Dentist?
If you notice your dental implant or the supported prosthesis has become loose, you should contact your dentist immediately for treatment. If the implant or supported prosthesis comes off (which is rare), you should preserve them and give them to your dentist during your next visit. In some cases, they may be reinserted without the need for surgery. If you observe bleeding, foul smell, redness, or swelling of the soft tissues around the implant site, these conditions should not be taken lightly, you should contact your dentists office right away.

Trevor Hart, DMD - General Dentist Kelly Cundy Hart, DMD - Board Certified Pediatric Dentist
We hope you enjoyed our 'Ultimate Guide to Dental Implants' and that it helped educate you on the topic of implant dentistry.
If you are interested in getting a Dental Implant in Fort Lauderdale, experience a comfortable experience with us. Our implant dentists and state-of-the-art facility will ensure a satisfactory outcome of your implant procedure.